Cardiovascular disease (CVD) remains a leading cause of morbidity and mortality worldwide, making its early diagnosis crucial in reducing complications and improving patient outcomes. With advancements in medical technology, healthcare providers now have access to a range of diagnostic tools that can accurately assess heart health. Understanding how cardiovascular disease is diagnosed involves recognizing symptoms, utilizing non-invasive and invasive testing methods, and interpreting the results to guide treatment. This article explores the comprehensive approaches used in the diagnosis of CVD, offering insight into the latest advancements and clinical protocols designed to detect heart disease effectively.
You may also like: 5 Modern Treatments for Heart Disease: Advancements in Cardiac Care
Recognizing the Early Signs of Cardiovascular Disease
The diagnosis of CVD often begins with identifying key symptoms that may indicate underlying heart problems. While some individuals may experience obvious warning signs such as chest pain, shortness of breath, or palpitations, others may have silent or atypical symptoms that complicate early detection. Fatigue, dizziness, swelling in the legs, and unexplained weakness can also suggest cardiovascular issues. In some cases, symptoms appear only during physical exertion, while in others, they occur unpredictably at rest.
Understanding risk factors is another crucial aspect of early detection. Patients with hypertension, diabetes, high cholesterol, obesity, or a family history of heart disease should undergo routine cardiovascular evaluations. Lifestyle choices such as smoking, poor diet, and physical inactivity further elevate the risk of developing heart-related conditions. Primary care physicians and cardiologists consider these factors when deciding whether further diagnostic testing is necessary.
Physical Examination and Medical History Review
A comprehensive medical history and physical examination serve as the foundation for diagnosing cardiovascular disease. Physicians begin by assessing a patient’s overall health, focusing on past illnesses, genetic predisposition, and lifestyle habits. Questions about chest pain, breathing difficulties, dizziness, and exercise tolerance help clinicians determine the likelihood of underlying cardiovascular problems.
During a physical examination, doctors measure blood pressure, check for irregular heartbeats, and listen for abnormal heart sounds using a stethoscope. They also examine the skin for signs of poor circulation, such as discoloration or cold extremities, and assess the presence of swelling, which may indicate fluid retention due to heart failure. In addition, evaluating peripheral pulses can reveal potential arterial blockages or circulation issues.
Electrocardiogram (ECG/EKG)
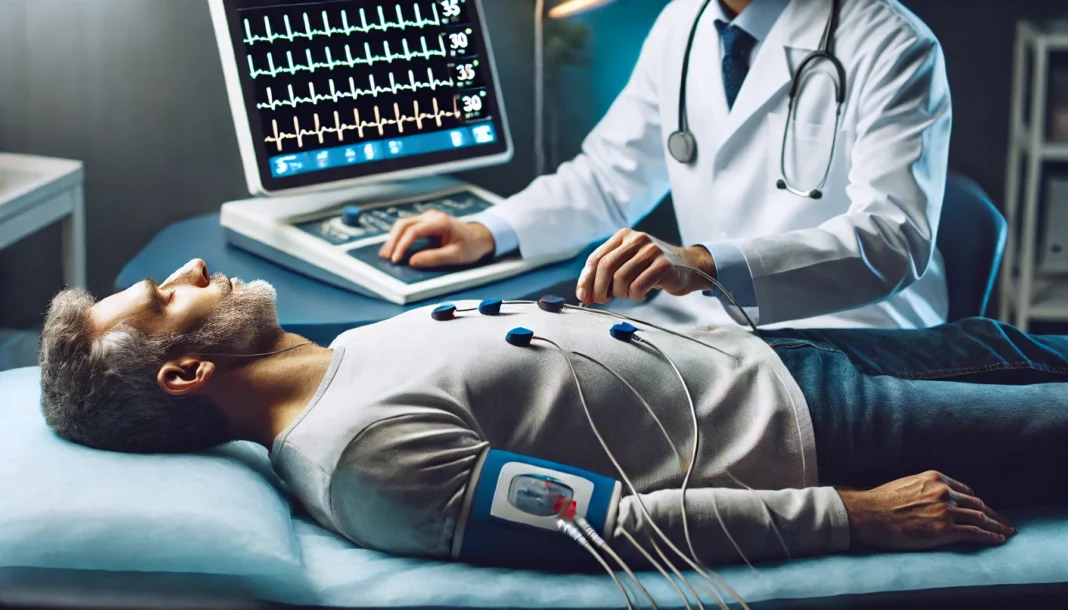
One of the most commonly used tests for diagnosing heart disease is the electrocardiogram (ECG or EKG). This non-invasive test records the electrical activity of the heart and provides essential information about heart rhythm, conduction abnormalities, and ischemic changes. An ECG can detect arrhythmias, previous heart attacks, and conditions such as atrial fibrillation, which increases the risk of stroke.
In clinical practice, a standard 12-lead ECG is often performed as an initial screening tool. If abnormalities are detected, additional ECG variations, such as a stress ECG or Holter monitoring, may be recommended. A stress ECG evaluates heart function under exertion, while a Holter monitor provides continuous ECG recordings over 24 to 48 hours to capture irregularities that may not appear during a short examination.
Echocardiography: Assessing Heart Structure and Function
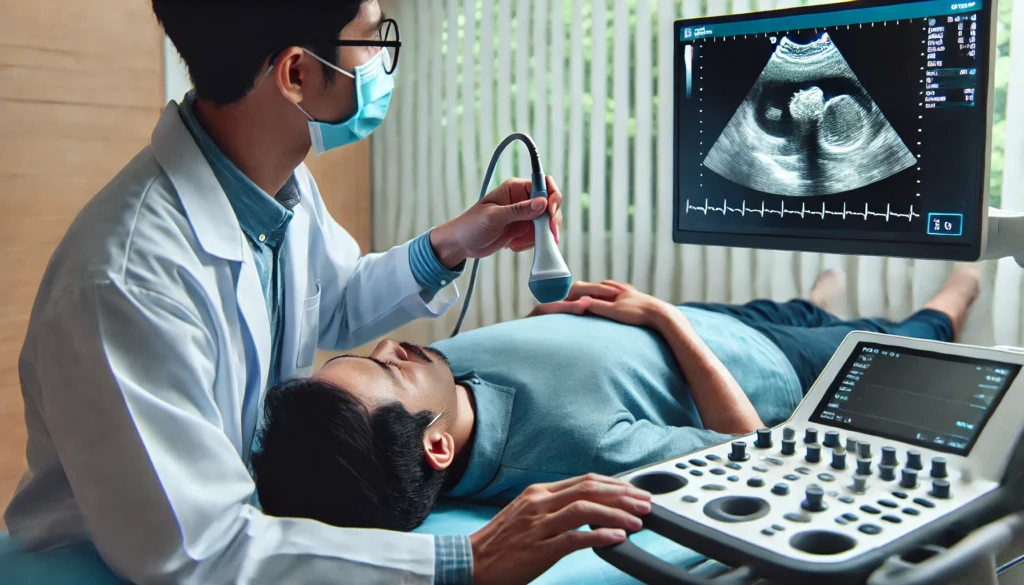
Echocardiography is another essential diagnostic tool that provides real-time imaging of the heart using ultrasound waves. This test helps evaluate heart structure, chamber size, valve function, and overall cardiac performance. It is particularly useful in detecting conditions such as heart failure, cardiomyopathy, and valvular diseases.
There are different types of echocardiography, each serving specific diagnostic purposes. Transthoracic echocardiography (TTE) is the most commonly used form, involving an ultrasound probe placed on the chest. Transesophageal echocardiography (TEE) offers more detailed images by inserting a probe into the esophagus, allowing for clearer visualization of the heart’s posterior structures. Stress echocardiography assesses heart function under physical or pharmacologic stress, helping detect ischemic changes indicative of coronary artery disease.
Stress Testing: Evaluating Heart Performance Under Exertion
Stress testing plays a critical role in diagnosing cardiovascular disease by measuring the heart’s response to increased workload. During a treadmill or bicycle stress test, a patient exercises while connected to an ECG, and changes in heart rate, blood pressure, and electrical activity are monitored. This test helps identify exercise-induced arrhythmias and ischemic changes that suggest blocked arteries.
For patients who cannot engage in physical exercise, pharmacologic stress tests use medications such as dobutamine or adenosine to stimulate heart activity artificially. These tests provide valuable insights into coronary circulation and myocardial function, especially when combined with imaging techniques like echocardiography or nuclear perfusion scans.
Advanced Imaging Techniques for Detecting Heart Disease
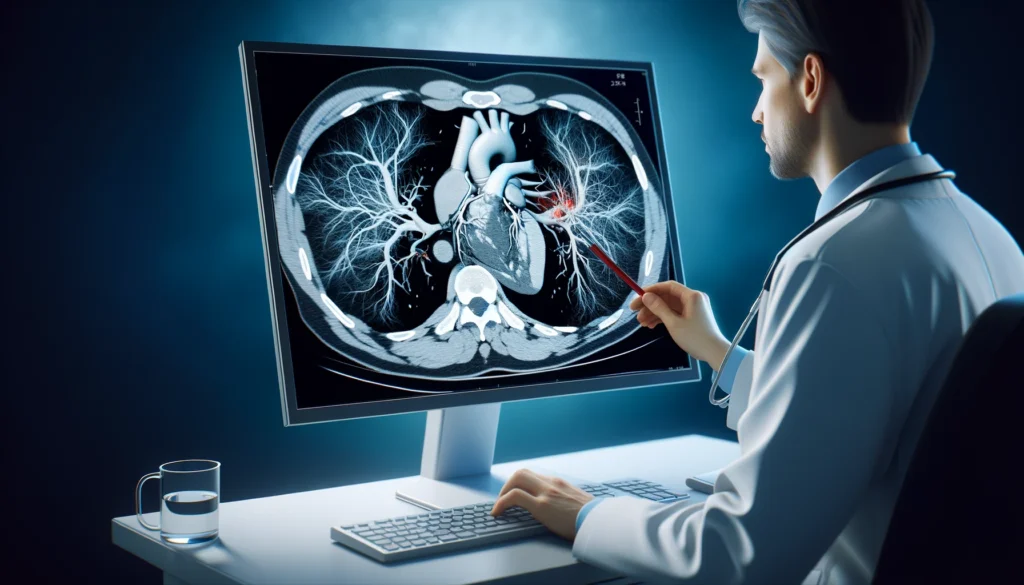
Beyond traditional diagnostic tests, advanced imaging techniques have revolutionized the early detection of cardiovascular disease. Coronary artery calcium (CAC) scoring, performed using computed tomography (CT), helps assess the presence and extent of calcified plaques in the coronary arteries. This test is particularly useful for identifying asymptomatic individuals at risk of heart disease.
Cardiac magnetic resonance imaging (MRI) offers high-resolution images of the heart’s structure and function, making it a valuable tool for diagnosing congenital heart disease, myocarditis, and fibrosis. Similarly, cardiac computed tomography angiography (CCTA) provides detailed images of coronary arteries, allowing clinicians to detect narrowing or blockages with high precision.
Laboratory Tests and Biomarkers in CVD Diagnosis
Blood tests play a vital role in diagnosing and monitoring cardiovascular disease. High levels of cholesterol, triglycerides, and inflammatory markers such as C-reactive protein (CRP) indicate an increased risk of atherosclerosis. Additionally, tests measuring levels of troponin, a protein released during heart muscle damage, are essential for diagnosing acute myocardial infarction.
Other biomarkers, such as B-type natriuretic peptide (BNP), help assess heart failure severity, while glucose and hemoglobin A1c levels provide insights into diabetes-related cardiovascular risks. Routine blood tests combined with imaging studies offer a comprehensive approach to evaluating cardiovascular health.
Frequently Asked Questions (FAQ) on Cardiovascular Disease Diagnosis
1. What are the latest advancements in the diagnosis of CVD? The diagnosis of CVD has evolved significantly with the integration of cutting-edge technologies such as artificial intelligence (AI), machine learning, and advanced imaging techniques. AI-powered algorithms now assist in analyzing electrocardiograms (ECGs) and imaging scans, allowing for more accurate and faster detection of abnormalities. Additionally, wearable devices equipped with real-time ECG monitoring help detect irregular heart rhythms and provide early warnings of potential heart disease. Genetic testing is also gaining traction, enabling physicians to assess hereditary risks and predict cardiovascular conditions before symptoms arise. These innovations collectively improve how cardiovascular disease is diagnosed, leading to more personalized and proactive healthcare.
2. How can genetic testing help in the diagnosis of CVD? Genetic testing plays a crucial role in identifying individuals at high risk of developing cardiovascular disease. By analyzing specific gene mutations associated with inherited heart conditions, such as hypertrophic cardiomyopathy and familial hypercholesterolemia, physicians can detect heart disease before symptoms appear. Genetic profiling can also help determine an individual’s response to medications, allowing for more tailored treatment plans. Family members of those diagnosed with hereditary cardiovascular diseases can benefit from early screening and preventive interventions. As research progresses, genetic testing is becoming a more accessible and integral tool in how CVD is diagnosed.
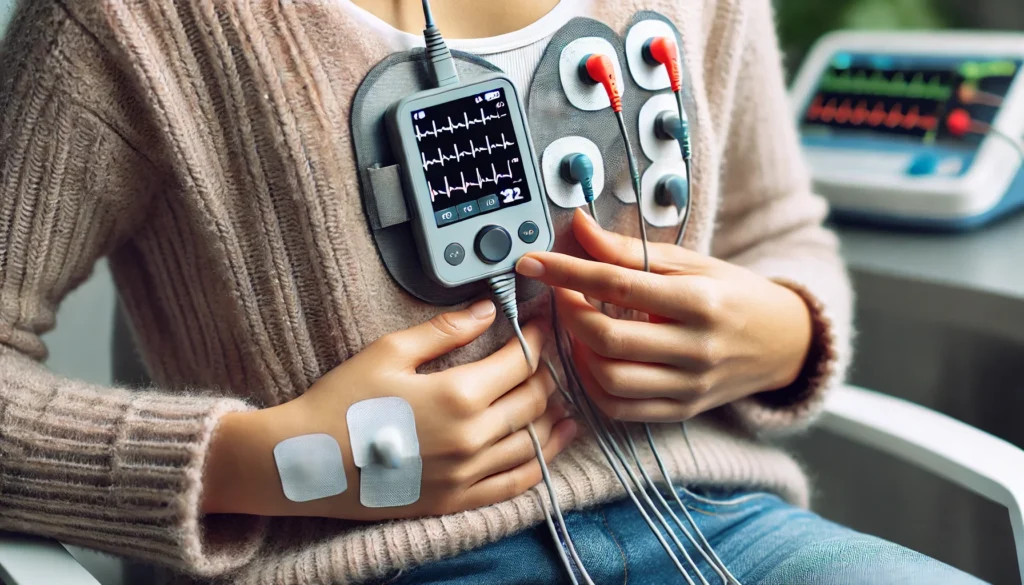
3. What role do wearable health devices play in detecting heart disease? Wearable technology, such as smartwatches and fitness trackers, has revolutionized how to detect heart disease by providing continuous heart rate and ECG monitoring. These devices can identify irregular heart rhythms, such as atrial fibrillation, and alert users to seek medical evaluation. Some advanced models also measure oxygen saturation levels and detect abnormal variations in heart rate, which can be early signs of cardiovascular issues. By integrating real-time health tracking with mobile applications, individuals can share their health data with their healthcare providers for more comprehensive assessments. Wearables serve as an important early warning system, complementing traditional diagnostic methods.
4. How does inflammation contribute to cardiovascular disease, and can it be measured? Chronic inflammation is increasingly recognized as a major contributor to cardiovascular disease, with elevated levels of inflammatory markers linked to a higher risk of heart attacks and strokes. High-sensitivity C-reactive protein (hs-CRP) testing is one method used in the diagnosis of CVD to measure systemic inflammation levels. Other inflammatory biomarkers, such as interleukin-6 and fibrinogen, also provide valuable insights into vascular health. Lifestyle factors like poor diet, stress, and smoking can exacerbate inflammation, making it essential to monitor these markers in at-risk individuals. Detecting and managing inflammation early can play a key role in preventing cardiovascular complications.
5. Can artificial intelligence improve the accuracy of cardiovascular disease diagnosis? Artificial intelligence is transforming how cardiovascular disease is diagnosed by enhancing the interpretation of medical imaging, ECGs, and patient data. AI-driven algorithms analyze vast amounts of clinical data to identify patterns that may be missed by human interpretation, leading to earlier and more precise diagnoses. Machine learning models can also predict the likelihood of heart disease progression, enabling proactive treatment plans. AI applications in radiology help improve the detection of arterial blockages through automated image analysis. As AI continues to evolve, it will play an increasingly vital role in refining how to diagnose heart disease with greater speed and accuracy.
6. How effective are coronary artery calcium (CAC) scans in predicting heart disease? Coronary artery calcium (CAC) scans have emerged as a valuable tool in assessing an individual’s risk for developing cardiovascular disease. This non-invasive imaging test detects calcium deposits in the coronary arteries, which are indicative of atherosclerosis. Higher CAC scores correlate with an increased likelihood of heart attacks and other cardiac events. Physicians use CAC scoring as part of a comprehensive approach to risk stratification, particularly for individuals with borderline cholesterol levels or a family history of heart disease. As CAC scans become more widely utilized, they enhance how is CVD diagnosed by providing a clearer picture of arterial health.
7. Can stress tests accurately detect hidden cardiovascular conditions? Stress tests are a fundamental component of how to diagnose heart disease, particularly in patients who experience exertion-related symptoms. These tests evaluate heart function under physical or pharmacological stress, identifying ischemia and arrhythmias that may not be apparent at rest. While traditional treadmill stress tests provide valuable insights, combining stress tests with imaging techniques, such as echocardiography or nuclear scans, enhances diagnostic accuracy. However, stress testing alone may not detect early-stage coronary artery disease, necessitating complementary assessments like coronary CT angiography. The integration of stress testing with advanced imaging improves how cardiovascular disease is diagnosed by offering a more comprehensive evaluation.
8. Are there any emerging blood biomarkers for detecting heart disease? The search for novel blood biomarkers is transforming how to detect heart disease with greater precision. Beyond traditional markers like troponins and cholesterol levels, researchers are exploring additional indicators such as myeloperoxidase (MPO), galectin-3, and microRNAs. These biomarkers provide insights into oxidative stress, fibrosis, and endothelial dysfunction, all of which contribute to cardiovascular disease. Early detection of such markers allows for more targeted interventions and preventive measures. As biomarker research advances, routine blood tests may soon include more sophisticated indicators to refine how is CVD diagnosed.
9. How does sleep quality affect cardiovascular disease risk and diagnosis? Sleep disturbances, including sleep apnea and insomnia, have been strongly linked to cardiovascular disease. Poor sleep quality can contribute to hypertension, inflammation, and metabolic disorders, all of which increase the likelihood of heart problems. Advanced sleep studies, such as polysomnography and home-based monitoring, help detect sleep-related cardiovascular risks. Many patients with undiagnosed heart disease exhibit abnormal heart rate variability during sleep, prompting further cardiovascular evaluations. Recognizing the interplay between sleep and heart health has become an important aspect of how to diagnose heart disease more holistically.
10. What future developments can improve the diagnosis of cardiovascular disease? Future advancements in medical technology and precision medicine will continue to refine how cardiovascular disease is diagnosed. Innovations such as lab-on-a-chip devices, which enable real-time blood analysis, could make early detection more accessible. Non-invasive molecular imaging techniques are being developed to visualize plaque stability, providing insights into stroke and heart attack risk. Additionally, integrating electronic health records with AI-powered predictive analytics will allow for more personalized and data-driven diagnosis. As these advancements progress, how to detect heart disease will become increasingly efficient, improving early intervention and patient outcomes.
Conclusion: The Importance of Early Diagnosis and Comprehensive Assessment
Early and accurate diagnosis of cardiovascular disease is fundamental to preventing complications and improving long-term health outcomes. By integrating medical history, physical examinations, and advanced diagnostic techniques, healthcare professionals can detect heart disease at its earliest stages and develop targeted treatment strategies. As medical technology continues to evolve, the future of cardiovascular diagnostics promises even greater precision, enabling timely interventions and better patient care. Understanding how to diagnose heart disease remains a critical component of modern medicine, ensuring that individuals at risk receive the necessary evaluations to maintain heart health.
heart disease screening, early heart disease detection, cardiovascular health tests, coronary artery evaluation, heart rhythm assessment, echocardiogram analysis, stress test for heart, cardiac biomarkers, inflammation and heart disease, AI in cardiology, non-invasive heart tests, coronary calcium scan, heart disease prevention strategies, advanced cardiac imaging, wearable heart monitors, genetic risk for heart disease, diagnosing heart conditions, heart attack risk factors, blood tests for heart health, cardiac MRI scan
Further Reading:
Disclaimer
The information contained in this article is provided for general informational purposes only and is not intended to serve as medical, legal, or professional advice. While MedNewsPedia strives to present accurate, up-to-date, and reliable content, no warranty or guarantee, expressed or implied, is made regarding the completeness, accuracy, or adequacy of the information provided. Readers are strongly advised to seek the guidance of a qualified healthcare provider or other relevant professionals before acting on any information contained in this article. MedNewsPedia, its authors, editors, and contributors expressly disclaim any liability for any damages, losses, or consequences arising directly or indirectly from the use, interpretation, or reliance on any information presented herein. The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the official policies or positions of MedNewsPedia.